Patients with impaired mobility are especially susceptible to pressure injuries,
sometimes called bed sores. These painful injuries develop when there is unrelieved pressure to the skin, reducing blood flow to the area.
Each year, it’s estimated that 2.5 million patients in U.S. acute-care facilities suffer from
pressure injuries, according to the Agency for Healthcare Research and Quality. What’s more, patients who develop pressure injuries in the hospital are more likely to have longer stays and a higher risk of death and readmission within 30 days of discharge.
To help improve patient safety and clinical outcomes, Trinity Health, parent organization of St. Francis Medical Center, has provided St. Francis with a grant to replicate the Patient Monitoring System, manufactured by Smith+Nephew, that was successfully piloted by a sister hospital within Trinity Health. Maria Sbarro, BSN, RN, CWCA, wound care coordinator at St. Francis, said, “The LEAF Patient Monitoring System is a great tool to help ensure timely and accurate repositioning of our high-risk patients. It also saves staff time.”
Hospitals using the LEAF Sensor technology have reported significant improvements in
adherence to patient turning protocols and reductions in hospital-acquired pressure injuries by as much as 85 percent.
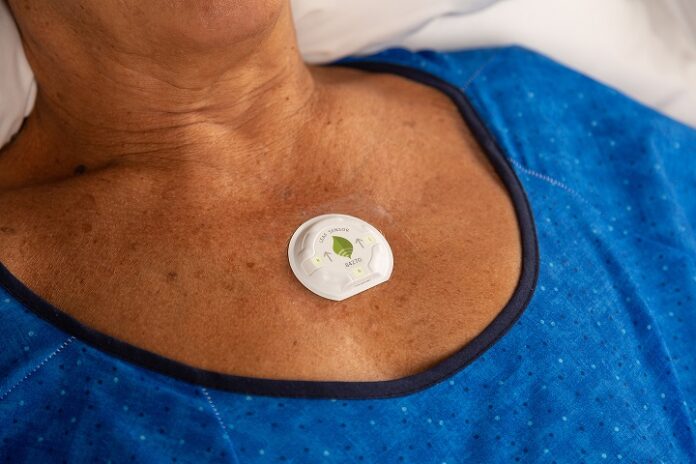
The lightweight, disposable LEAF Sensor is placed on the patient’s chest. Its triaxial
accelerometer then automatically measures the patient’s position, orientation and activity and wirelessly transmits the data to monitoring stations easily viewed by clinical staff.
The LEAF system provides visual alerts to staff so patients are repositioned according to their individually prescribed turning schedule, and confirms adequate pressure reduction is achieved with each turn. The sensor registers independent patient movement and automatically adjusts the schedule accordingly, saving staff time when patients reposition on their own.
Alerts can also be set to help prevent repositioning patients on an existing wound or an area of concern. In addition, the system provides various levels of reporting to help with root cause analysis and improve care delivery.
Traditional measures for preventing pressure injuries include daily skin inspections,
repositioning a patient every two hours, padding bony prominences and using specialized
mattresses to reduce/redistribute pressure. However, even with traditional measures, some patients remain at-risk for pressure injuries. These include: patients over the age 70 (due to aging skin, greater risk for hardening of the arteries and poor circulation); patients with multiple medical diagnoses; patients with health conditions such as paralysis after stroke or other diseases that make mobility difficult and/or affect sensation (the ability to feel pressure); patients with poor nutrition or malnourishment; and patients with type 2 diabetes, who have damage to their blood vessels that makes blood flow slow and obstructed.
“I am very excited we have been given this opportunity to implement the Leaf Sensor system at St. Francis,” said Sbarro. “It will help improve patient safety and care.”